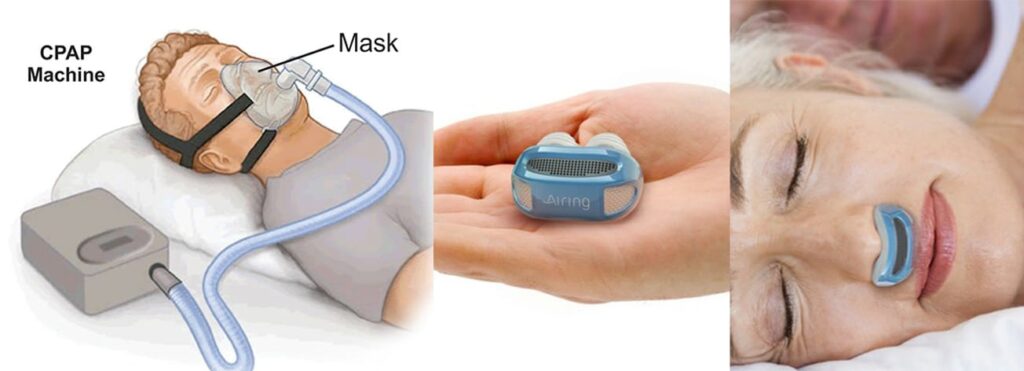
Use of CPAP works wonders in most patients who have obstructive sleep apnea. In this, through a snugly fitting face mask, air is blown into the nostrils to keep the airway open during sleep. Oxygen may be required in some cases in addition to the air under pressure. Tongue-retaining devices or bite guards can be used to bring the lower jaw forward and thereby alleviate posterior airway obstruction during sleep. Weight loss of even 10% can eliminate apneic episodes by reducing the mass of the posterior airway. If there are associated anatomic deficits in the jaw, this alone might not help.
Weight loss surgery in morbidly obese patients with obstructive sleep apnea is a very good option. Remarkable results are seen with loss of the first 10 to 15 kgs. The results may be due to a reduction in the adipose level of parapharyngeal tissues. Once all the excess weight is lost after weight loss surgery, there is complete remission for sleep apnea. The surgery of choice is the Roux en Y gastric bypass, however, the sleeve surgery could also be an option. The results are very dramatic, the person can sleep well at night without any snoring, disturbance of waking up. When the person wakes up in the morning, there is no headache, no dryness of mouth and they feel fresh (the freshness they have not experienced over years). They don’t fall asleep while talking to people or while driving at a traffic signal.
Uvulopalatopharyngoplasty involving removal of part of the soft palate, uvula and redundant peripharyngeal tissues, sometimes including the tonsils could be effective in eliminating snoring; however, it is not necessarily curative for obstructive sleep apnea, because areas of the airway other than the soft palate also collapse in most patients with this sleep disorder.
Jaw surgery for a retrognathic mandible. The surgical procedure could entail genioplasty or moving both the mandible and maxilla. In noncompliant patients with extremely severe apnea, tracheostomy may be considered.